Online Courses
"Your Educational Journey Starts Here"Cardiac Arrhythmia Interpretation
View Course
Atrial Arrhythmias
The presence of atrial fibrillation alters cardiac function and places the patient at risk for stroke. Effective management and patient education requires knowledge of rate and rhythm control strategies and an understanding of stroke risk and prevention options. This course provides an overview of the comprehensive management of atrial fibrillation including pharmacological and non-pharmacological strategies. In addition to atrial fibrillation, the nuances of atrial flutter will also be presented.
Please Note: This course was recorded as part of the Cardiac Rhythm Management course and is being offered as an individual CE offering for those not purchasing that course.

View Course
AV Blocks & AV Dissociation
AV blocks are among the most confusing arrhythmias encountered in clinical practice. This class presents an updated classification system for AV blocks and discusses in detail the following AV blocks: First Degree, Second Degree, Type I, Second Degree, Type II, High Grade Block and Third Degree Block. Ladder diagrams are used to illustrate rhythm strips, and instructions for constructing ladder diagrams and using them as a teaching aid are presented. The four causes of AV dissociation are presented along with examples of each.
View Course
Bedside Cardiac Monitoring
This Cardiac Monitoring course provides knowledge and skills that bring bedside monitoring practice into alignment with the evidence-based practice guidelines published by the American Heart Association and the Practice Alerts on ST Segment Monitoring and the Dysrhythmia Monitoring published by the American Association of Critical Care Nurses. This short course covers the 3 primary purposes for bedside cardiac monitoring: arrhythmia detection, QT interval monitoring and ST segment monitoring. You will develop an understanding of how you can best use the bedside monitor to help you care for your patient. From when and why to use different leads to how to better set your alarms to eliminate nonactionable alarms and assure appropriate alarm notification so you don’t miss key changes. Throughout the course you will learn tips and tools that will enhance your use of the bedside monitor. This will help improve patient outcomes and your confidence in the care of patients on cardiac monitoring. Case examples are used to demonstrate the clinical impact of cardiac monitoring utilization that is evidence based.
View Course
Cardiac Arrhythmias and Monitoring Short Course
Are you new to Arrhythmia interpretation? Great, this course is just for you. This short course provides the learner with the fundamental knowledge required for accurate arrhythmia Interpretation. Topics include AV blocks, bundle branch blocks, tachycardias, atrial fibrillation, supraventricular tachycardias, ventricular tachycardias, and Torsades de Pointes. You will finish this course with practical information to immediately apply in your practice.

View Course
Cardiac Arrhythmia Interpretation: Essential Skills for Clinical Practice (For Nurses)
This course provides the basic knowledge and skills needed to interpret cardiac arrhythmias in any setting and is appropriate for nurses, monitor technicians, EMS personnel, and medical students. Content includes: principles of cardiac anatomy and physiology related to the origin and electrical activation of the heart during normal and abnormal cardiac rhythms, an organized 5-step approach to rhythm interpretation, descriptions of each cardiac rhythm with examples and practice strips to reinforce learning, practice sessions and homework related to each topic area. Pharmacologic and electrical therapy is included for rhythms requiring treatment. The emphasis in this course is on rhythm strip interpretation and appropriate treatment for life-threatening arrhythmias.
“Carol’s rate and rhythm of speaking were so smooth and easy to understand. The diagrams used in time with the verbal explanations helped me get a better picture of what Carol was describing. I learned so much from this course, will recommend it to peers.” — D.F.
“Very well structured and quite easy to follow. The homework and ECG strips are essential to revise and assess one’s learning throughout the course. Highly recommended.” — C.X.
“I love this course! giving me so much info with well-organized topics and detailed explanations and also strips to be analyzed. The instructor, Carol, is amazing!“
View Course
Cardiac Arrhythmia Management: Beyond the Basics
This course will sharpen your rhythm interpretation skills and give you certainty in response to a change in your patient’s cardiac rhythm. This is a comprehensive rhythm management course taking you beyond the basics in arrhythmia recognition and management. The course will take a deeper dive into recognizing bradycardias and heart blocks, atrial fibrillation, narrow and wide complex SVTs, and prolonged QT disorders that will strengthen your current knowledge. The course is appropriate for advanced practice nurses, nurses, and monitor technicians who want to expand their current knowledge of cardiac arrhythmias in adult patients beyond the basics.
Prerequisite knowledge: Basic understanding of cardiac conduction and basic arrhythmia interpretation (P waves, QRS complexes, normal intervals).
Please Note: This course is part of the Institute of Excellence in Cardiovascular Essentials Learning Plan and the Advanced Practice Package.
View Course
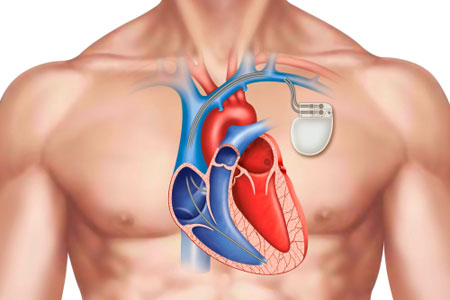
Pacemakers and Implantable Cardioverter Defibrillators
This program is for nurses and other health care professionals in telemetry/step-down units, critical care, emergency departments, and other settings who care for patients with temporary or permanent cardiac pacemakers or implantable cardioverter defibrillators (ICD). Content includes: indications for pacing, basic pacemaker operation, single and dual chamber pacemaker function, single and dual chamber pacemaker evaluation for capture and sensing, rate adaptive pacing, special features of dual chamber pacemakers, cardiac reynchronization therapy with biventricular pacing and His bundle pacing, pacing modes to reduce unnecessary right ventricular pacing, ICD function, and patient care after implantation. Content does not include pacemaker programming.
View Course
Supraventricular Tachycardias
Supraventricular tachycardias are commonly encountered in clinical practice. Sometimes understanding and differentiating these arrhythmias can be confusing. This class discusses AV nodal passive and AV nodal active tachycardias, ECG clues to identify them, and their treatment. Atrial fibrillation is not included since there is a separate class on that topic.
Arrhythmias covered include:
- Sinus tachycardia
- Atrial tachycardia
- Multifocal atrial tachycardia
- Atrial flutter
- AV nodal reentry tachycardia
- AV reentry tachycardia using an accessory pathway

View Course
Wide Complex Tachycardias
Wide complex tachycardias occur frequently in the critical care setting. Differentiating VT from SVT is a skill that available to the nurse in the critical are unit. This class presents the most useful ECG and clinical criteria for making the differential diagnosis of wide QRS tachycardias. Content includes mechanisms of aberration and when to expect it, common cause of wide QRS tachycardias, best bedside monitoring leads and use of Lewis lead and atrial electrograms for rhythm identification, and the most useful ECG clues for differentiating wide QRS beats and rhythms. Emphasis is on the value of P waves, QRS morphology clues, fusion beats, QRS axis, and clinical clues to help you make an accurate interpretation of wide QRS beats and tachycardias.
Excellence Starts Here
Keep up-to-date with live classes, products, promotions, practice pearls and online courses.
Sign up today and receive a FREE GIFT, an exclusive offer available only to new subscribers.
Cardiovascular Nursing Education Associates
Exceptional Nurses, Exceptional Patient Care
